My Experience as a Student in Columbia University School of Nursing’s MDE/DNP Program
I have been a student in Columbia University School of Nursing’s (CUSON) Master’s Direct Entry (MDE) program since the summer of 2018 and will be continuing onto the Doctor of Nursing Practice- Psychiatric Mental Health (DNP-PMH) program in the fall of 2019. If everything goes according to plan, I’ll graduate from Columbia by the end of 2021 and fulfill my dream of helping people connect their mind, body, and purpose as a psychiatric nurse practitioner!
When I was trying to navigate my way through different direct-entry nursing programs, I remember being super confused and wishing that more students had posted their experiences in each program online. Here are the factors that most contributed the my initial decision to study at CUSON and to my experience thus far in the MDE program.
Location:
Columbia’s Morningside and Medical Campuses:
When I envisioned going to Columbia, I pictured spending long nights on marble steps, studying in the glow of Butler Library. My background music would consist of the hum of philosophy students debating a piece by Nietzsche, business students talking about their latest networking event, and medical students sharing the highlights of their latest clinical rotation would be my background music. Free time would be spent attending the hundreds of university or student-run events in and around Morningside Heights, Harlem, and the Upper West Side or exploring the neighboring part of Central Park. However, most of Columbia’s graduate-level health science programs are located on Columbia University Medical Campus (CUMC), located between 168th Street-175th Street and Broadway up in Washington Heights. This is important to bear in mind because Washington Heights is at least a decent half-hour commute from the Morningside campus by public transportation, making attending the many exciting talks and events hosted by Columbia College and Columbia’s other graduate schools harder (especially now that the 1-train is no longer stopping at 168th Street). CUMC has it’s own small library that is open 24/7, a basic gym, and nice facilities to study in (The Vagelos Education Center, Hammer Health Sciences Building, The School of Nursing), but it’s very much its own campus that feels isolated rather than integrated with the rest of Columbia University. There is still a host of engaging events, from networking sessions and alumni panels, to interdisciplinary talks and guest speakers at CUMC but the events mainly revolve around the health sciences. You will bump into a mix of students studying medicine, physical therapy, dentistry, public health, and nursing, but you’ll have to go to Morningside to meet graduate students in other fields. While the Morningside Campus has a very campus-y vibe, CUMC has its own unique vibe, with the integration of a large Dominican population mixing with a historically Irish-American population and the slew of young-professionals and health-science students from CUMC. So while CUMC/Washington Heights wasn’t what I was expecting, I’ve grown to appreciate the vibrant community and experience up here.
TLDR: Columbia’s Morningside Heights Campus ≠ Columbia University Medical Campus (CUMC).
 What I had envisioned my future campus to be.
What I had envisioned my future campus to be.
New York City:
As for living in Manhattan, I feel like every one has to experience living in the Big Apple- at least for a short period of time. Cities are nothing new to me- I’ve lived in Boston, D.C., and Shanghai for various time spans before I found my way to New York. But even then, New York is the “city-est” city I’ve ever called home. The sky scrapers are taller and more crowded than those in Boston and D.C., and the population is more diverse than those of the other 3 cities. The size and complexity of the metro-system in New York makes even an experienced daily public-transportation commuter in other cities confused for the first 2 weeks. A fast yet coordinated dance occurs on the narrow side walks, with a rush of busy New Yorkers quickly side-stepping impressively high trash piles, artists/musicians/performers, and lost, selfie-snapping tourists. There are literally hundreds of thousands of events to check out all day, every day. Like museums? You could spend months exploring every single museum in New York. Are you a foodie? You’re in the right place with 5 borough’s of food from every continent and at every price range. Enjoy hiking? There are a ton of trails available through public transportation with a trip on the Metro-North. For longer trips, you can drive a few hours north to the Catskill, Blackhead, or Adirondack Mountains in upstate New York. New York City is also on most everyone’s itinerary at some point- from famous speakers, musicians, and authors, to friends and family members from other areas of the nation or the world. I’ve bumped into people from all different time periods and geographic locations in my life in New York. Being in New York also makes it easier for me to have cheap and easy access to my friends and family in Boston, Philly, Connecticut, and D.C. with a <5 hour bus trip.
In terms of weather, I grew up near Boston, Massachusetts, so I was used to slightly chilly falls (40-60 degrees Fahrenheit), long/dark/cold/snowy winters, non-existent/rainy springs, and “hot” summers (above 80 degrees is too hot for me). When I was living in D.C., I found it both pleasantly and absurdly warm in the fall/spring (60-70’s!), temperate in the winter (20’s-50’s), and disgustingly hot/humid in the summer. New York falls right between these, feeling slightly muggier/hotter than Boston in the summer, temperate in the fall, occasionally cold in the winter (sometimes it’s below 20 with windchill), and we’ll see about the spring. People who aren’t from the Northeast may have to adjust to cooler temperatures and darker, longer winters than they’re used to. I’ve found Manhattan to be more cloudy/foggy than Boston and D.C., which is something to keep in mind if you struggle with Seasonal Affective Disorder or just love sunny weather!
TLDR: This is all to say that I’ve loved living in NYC- it’s exciting and filled with people and opportunities. However, if you’re not one for the hustle and bustle and somewhat chaotic nature of NYC, you might find another city more comfortable.
Columbia’s Master’s Direct Entry (MDE) Program:
This is a program for people who completed their Bachelor’s in another field and want to get into the field of nursing in a faster timespan than getting a 4-year BSN, and would like to take on leadership positions in nursing by also studying nursing at a Master’s level. You graduate with a Master’s of Science in Nursing and are eligible to take the NCLEX for your Registered Nurse (RN) license after completing this program.
Academics: When Columbia says that their Master’s Direct-Entry program is an accelerated program, they mean it. Think about it: you’re squeezing all the foundational nursing curriculum covered in a BSN, MSN curriculum, and clinical hours into 15 months. How exactly is this achieved? Well, for one, you need to come in having taken all the basic sciences at a bachelor’s level including statistics, anatomy and physiology 1 & 2, microbiology, and nutrition. All applicants also have to have a Bachelor’s degree, so applicants have already covered non-nursing core-curriculum required in most BSN’s. And thirdly, you’re taking 17-21 official credits per semester for 4 semesters straight. I say official because although 17-21 credits may seem manageable (about 6-7 classes worth) based on undergraduate courses, I definitely had a lot less time with this course load than with the same course load in undergrad. Apart from the classes and clinical hours listed on the official schedule, you have to account for the numerous group-project meetings, review-sessions, simulation-lab hours, study-sessions, and commutes home/to class/to various clinical sites that occur before/after classes. This makes actual “free time” a bit limited, and during which you also have to dedicate to doing work/studying for all of the classes/clinicals you’re in. Personally, I found a lack of energy to be more of an issue than a lack of time because the amount of time you dedicate towards doing work/studying is really up to you. I found myself having to choose between amount of time studying and amount of time socializing, exercising, cooking, cleaning, sleeping, reading, exploring the city, doing extracurricular activities, ect.
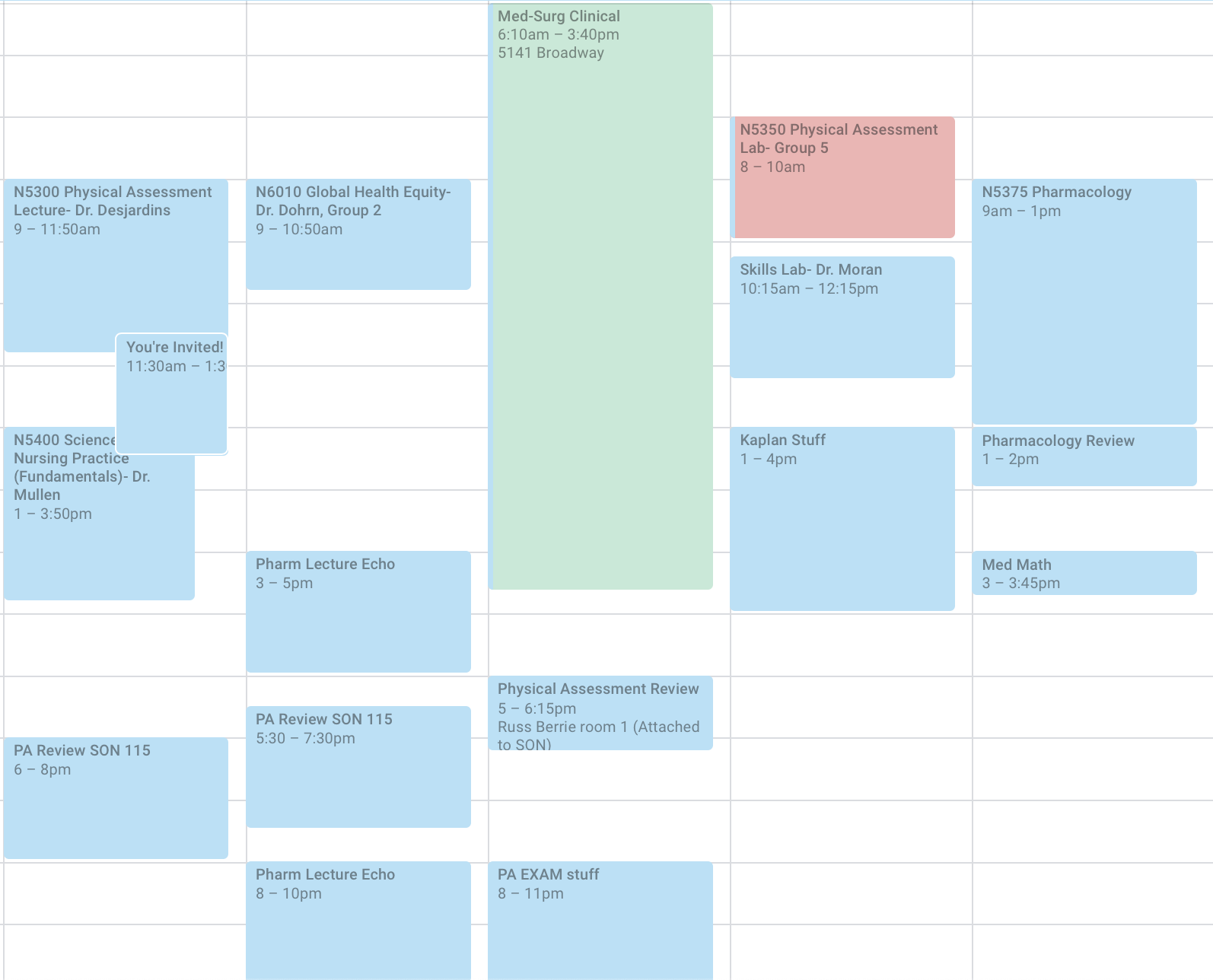
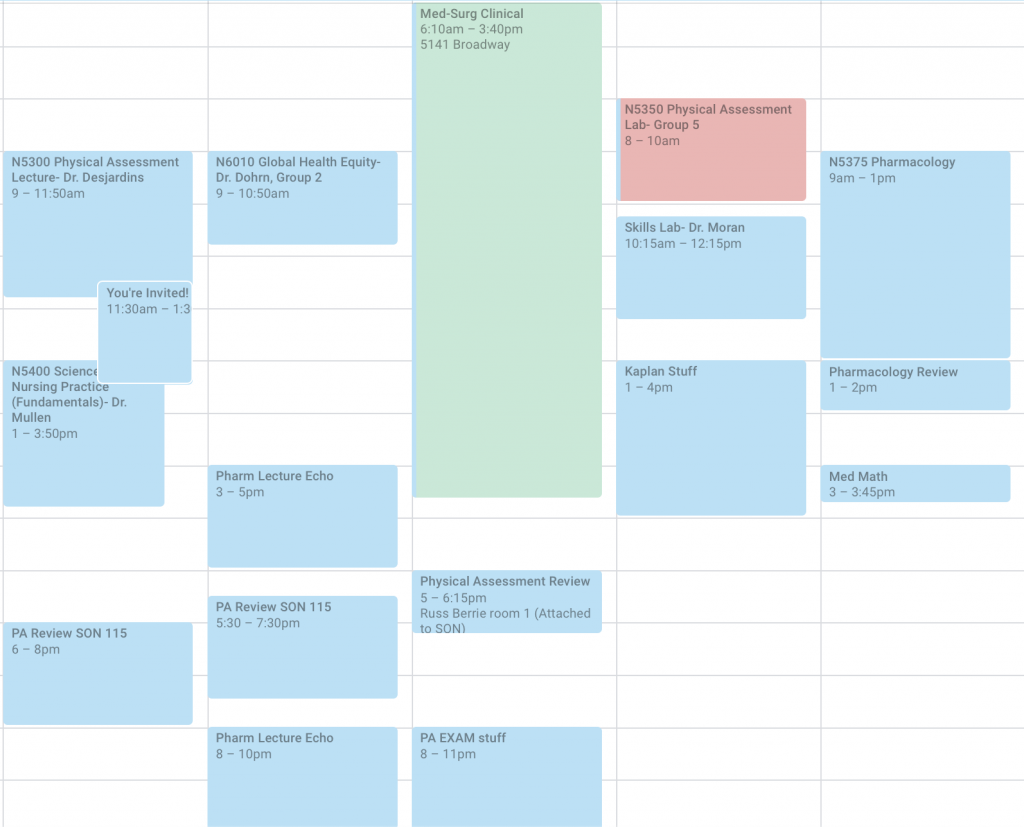
One week in my calendar during the first summer of MDE.
Would I say that classes are hard? Yes and no. I wouldn’t say that the material in any of the courses are necessarily hard conceptually. What is challenging is the amount of both conceptual material, hands-on skills, and clinical judgement skills you need to master and integrate in a very limited amount of time. If you did fine on your basic-science prerequisites, you are equipped to do well on the courses conceptually- you just need to focus on balancing your time, energy, mental health, and other obligations well (or in other words, connecting mind body and purpose 🙂 ).
Some classes are taught and received well (ex. many people like med-surge, pharmacology, pathophysiology, pediatrics, psych) and some are less-structured, not received well, or “fluff” courses. While I wish the latter were stronger courses, I also honestly needed some fluff courses to balance out the more time-consuming and challenging courses. Additionally, while didactic courses are important for establishing a foundational base of knowledge, I believe that a motivated and curious person can learn didactic material anywhere, so I personally place more importance on the quality of clinical learning than on classroom learning.
TLDR: Get ready to be busy. It’s the quantity, not quality of the material that is hard. Some courses are great, some are meh, but I think that didactic courses come secondary to clinical learning.
Clinicals: If I had to choose one strength of CUSON’s programs, it would be the clinical placements students have access to due to Columbia’s clinical affiliations/relationships. CUMC is directly affiliated with New York Presbyterian (NYP) (ranked as the 10th best hospital from 2018-2019 in the nation by US News and World Report) with its multiple branches (Children’s Hospital of New York, Weill Cornell Medical Center, Milstein Hospital, Allen Pavilion), and has connections to other major hospitals and health care facilities like Mount Sinai, Mount Sinai-St. Luke’s, New York State Psychiatric Institute, Nyack Hospital, and Montefiore Medical Center. Because NYP and Mount Sinai in particular are major hospitals located in a major city, you are exposed to unique and complex medical cases that you would be less likely to see at smaller hospitals. Because NYP is a large hospital with many specialized units in each segment of medicine, I’ve had the privilege of being placed on an oncology unit during my pediatrics rotation, and some of my classmates have been placed on neurology and cardiac-step-down units. There are also opportunities to shadow for a day in different hospital departments, like the Intensive Care Unit, Emergency Department, Gastroenterology, ect.
As I alluded to in the section above, I feel that actual face-to-face contact time with patients is the most valuable type of education one can get as a clinician. Anyone can memorize signs/symptoms and understand the pathophysiology of a disease, but I didn’t truly understand a disease until I was able to see and connect it with an actual patient and their story. Thankfully, in CUSON’s MDE program, they throw students right into clinical rotations in the 2nd week of the program! This was terrifying and exciting in equal parts, but it was only through being forced to immediately learn and apply clinical skills and concepts on the spot that I was really able to learn at the accelerated pace that the program demands. One question I get from a lot of prospective students is whether or not I felt “prepared” for clinicals. Honestly, no, I didn’t- I often felt uncomfortable in a new environment, dealing with unfamiliar conditions, and being under pressure to perform well at skills I had never done on a real person before. But that’s the point of clinical rotations. You’re there to learn and make mistakes while you still have support and guidance from the other students in your clinical group, your clinical instructor, and the nurses you’re working under at the medical facility. It’s only by jumping right into the clinical environment that get comfortable being uncomfortable, develop the thick skin you need as someone working directly with people, and learn to advocate for yourself and your education with your clinical instructors/nurses.
This is how clinicals work in the MDE Program:
1.) Summer 1: 8 weeks, once a week for 8 hours – (56 clinical hours total)
- Groups of 8-10 students with 1 clinical instructor
- You generally get paired with another student for the span of this clinical rotation so that you’re not alone
- Usually on a Med-Surge Floor (pre-operative, post-operative, and basic medical care for stable patients)
- Practicing basic nursing skills like bed baths/hygiene care, taking vitals, doing focused and full physical assessments, safety precautions (lowering/locking beds, making sure call bell is there, hand hygiene, personal protective equipment), building patient rapport, preparing/caring for patient rooms, giving/taking report from nurses, performing patient education
- Being introduced to more complex nursing skills like prioritization of patients, planning and organization tasks to be most time-efficient, learning when and how to communicate with various kinds practitioners in the medical team, understanding the impact, implications, and nursing interventions of symptoms and diseases on a patient’s health/quality of life, understanding how to analyze lab values, understanding what to check for in terms of medication (side-effects, contraindications, accurate dosages, administration, precautions)
- Getting introduced to and used to thinking in terms of nursing diagnoses (different than medical diagnoses-important to understand both)
- First concept-map: you take a patient you worked with and walk through the whole nursing process: assessment, diagnosis, outcome planning, implementation, and evaluation.
2.) Fall/Early Spring: 5 by 5 rotations– rotate through pediatrics, obstetrics, medical-surgical, psychiatric, and community nursing clinicals, which occur 2 days a week (8 hours/day) for 5 weeks each – (80 total clinical hours per rotation, 400 clinical hours total)
- Groups of 8-10 students with 1 clinical instructor
- Function independently (some clinical instructors pair you up during the first week)
- On floors of respective rotation, may be on specialized floors (oncology, neurological, cardiac)
- Do a concept map for each rotation except for psych in which you do a case-study
- Continue to use basic nursing skills and develop complex nursing skills
- Learn nursing skills specific to the rotation (ex. assessing fundus in OB, doing mental status exam in Psych, assessing developmental level of children in Peds, understanding the role of public and community health in health care in Community, integrating nursing skills together in Med-Surge)
- Community rotations are at various community sites in New York, from community health centers, schools, hospice/palliative care programs, nursing homes, homeless shelters, detox/withdrawal sites
3.) Late Spring: Integration– shadow a nurse preceptor full-time, three 12-hr shifts a week for 6 weeks – (216 total clinical hours)
- One-on-one with nurse preceptor (you’re doing a full-time nurse’s shifts with that nurse)
- Shifts may be at night
- If doing integration in New York, can be throughout 5-boroughs
- Option to do integration elsewhere, both domestically (Cooperstown in upstate New York, Alaska), and internationally (Dominican Republic, Ethiopia, Ghana, Jamaica, Jordan, Malawi, Mexico, Spain, Italy, India, China, Nepal). Sites are expanding and changing each year.
- You rank and are placed in one of the various specialties (ER, ICU, Adult/Gero, Pediatrics, Midwifery, Psych)
So in total, you complete about 352 clinical hours over the span of 39 weeks.
A question I’ve gotten from a few prospective students is whether or not I think that 8-10 students per clinical instructor is too many. I personally liked that ratio- I felt like I had enough space to get a sense of independence, but that I had help when I needed it. Keep in mind that you receive guidance from both your clinical instructor, as well as from the students in your clinical group, and the nurse whose patients you’re taking care of for the day.
TLDR: CUSON has great clinical placements. You’ll learn a lot and have a lot of clinical hours.
The Doctor of Nursing Practice (DNP) Program: This is a 2-2.5 year program after which you earn your Doctor of Nursing Practice (DNP) and function as a Nurse Practitioner (NP) in a specific specialty (acute, midwifery, psychiatric, pediatric, family). To become an NP, you need to be certified (earn a specific number of clinical hours and fulfill specific clinical competencies) and licensed (graduate with your degree and pass your boards). The DNP programs for each specialty differ from one another but generally consist of didactic courses, at least 1000 clinical hours, simulation labs and recorded practice with live actors, an intensive full-time clinical experience, and a peer-reviewed publication (research article, poster, presentation). People can go into the DNP seamlessly after the MDE program, or apply internally during MDE. Because I haven’t finished the MDE portion yet, I don’t have personal experience with the DNP programs. Each DNP program is run by a different director, has different instructors, has slightly different requirements, and can be slightly different in terms of timespan (I think that midwifery and psych are 2 years (6 semesters) while the other specialties may be 1 semester longer).
DNP programs are currently transitioning from a 1-year full-time residency format (in which students could try to find a full-time paid job that fulfilled residency criteria or be placed into an unpaid residency by Columbia) to a 1-semester “intensive clinical experience” (in which all students are placed into unpaid clinical positions by Columbia). During the intensive clinical experience, students gain experience working full-time in an NP capacity while trying to fulfill specific clinical competencies under the guidance of a clinical preceptor. In other words, the new model consists of Columbia placing all students into NP clinical experiences (in the same manner students are assigned for other clinical placements) at which students will work full-time for 1 semester (while occasionally meeting with their advisor), fulfill specific clinical competencies, and have the guidance and supervision of a clinical preceptor. It was communicated that if a student has a particular interest in being placed at a specific hospital (including any clinical placements out of state) or with a specific preceptor, they will need to work with their DNP program director ahead of time to see if that can be arranged. Supposedly, this transition from residency to intensive clinical experience was made after many students found it stressful and challenging to find a paid-residency program or position that met the DNP residency criteria within a short time-span, resulting in students not being able to graduate on-time. I can see why this might occur because getting a nursing/NP job can sometimes take a few months, with applications, replies, interviews, legal clearance, hospital specific certifications, and a hospital training period. Additionally, the change was also reportedly initiated because some students who did find full-time jobs for residency found it difficult to complete all the necessary competencies to graduate while also trying to fulfill all the responsibilities of actually caring for patients in their first real NP job.
Here is what I’ve heard about the DNP programs:
Acute: the smallest and most competitive of the DNP programs. Requires at least 1 year of RN experience, preferably in Critical Care before starting the DNP portion. For people thinking about switching to acute or applying internally during the MDE program, remember that it is quite competitive! I know that a handful of people who tried to do that this year were rejected.
Midwifery: second smallest program. I think midwifery students need to complete more clinical hours during their program before they’re able to function clinically in a Nurse-midwife capacity.
Psych: third smallest program (has been around 18-25 students in the past). This program tries approach mental health treatment holistically, and I’ve heard that there’s an emphasis in using psychotherapeutic techniques in conjunction with psychopharmacological treatments for mental health disorders. However, I’m not sure how in depth the program goes into specific training in different schools of psychotherapy (ex. CBT, psychoanalytic, humanistic). I’d guess that PsyD and PhD programs in clinical psychology would be more comprehensive if you’re looking to focus purely on psychotherapy.
Peds: larger program of about 40-50? students. I’ve heard that you either LOVE working in pediatrics or absolutely can’t do it due to the emotional nature of working with sick children.
Family: largest program of about 50-60? students. This seems to be the most flexible in terms of scope of practice/settings in which you are able to function as a future family NP (ex. I’ve heard of family NP’s who have worked in more acute settings like the ICU/cardiac units as well as functioning in more general primary care settings).
TLDR: Overall, I’ve heard good things about the DNP programs. The smaller programs seem to be quite tailored to individual student preferences (in terms of clinical experience/focus). There seems to be a strong clinical emphasis in each of the DNP programs, with students graduating with at least 1000 clinical hours.
Cost:
This is one of the most expensive direct-entry nursing programs in one of the most expensive cities. Though Columbia’s Psych-DNP program was my top choice, I spent an entire month of sleepless nights agonizing over whether or not to accept my spot due to the astronomical cost.
MDE Cost: As of the summer of 2019, flat rate tuition for full-time students in the MDE portion is $27,680 per semester, with a projected 3% increase for the fall and spring terms. Don’t forget the cost of the last summer semester in the MDE program- it’s not shown in the tuition/fee calculations on the website.
Let’s do the math: 27,680 + 1.03($27,680)+ 1.03($27,680) + 1.03($27,680) = summer 1 tuition + fall tuition + spring tuition + summer 2 tuition = $113,211.20
Total number of credits taken in the program is around 72 credits. This means that you are paying over $1572 per credit. This is in 2019, and we all know prices only go up.
To be fair, other comparable direct-entry/accelerated nursing programs are also expensive. Other programs’ 2018-2019 accelerated BSN or direct-entry master’s level tuition rates:
Emory= $1,871/credit (for 120 credits of the accelerated BSN + MSN programs)
John’s Hopkins= $1,639/credit (for their 72 credit direct-entry MSN program)
UPenn= $117,850 total tuition (for the accelerated BSN program, they don’t break it down by credit hour online)
Boston College= $1404/credit (for the 77 credit direct-entry MSN program)
Mass General Institute of Health Professions = $1260/credit (for the 54 credit accelerated BSN)
DNP Cost: The website says that tuition for each year of the DNP is nearly $42,000/year. With recent changes, DNP programs may be 2 years or 2 years + 1 semester, with the final semester in the latter time span being charged at part-time rate and consisting of around 5 credits (which is considered part-time). I’m not sure exactly how much the part-time tuition is but I heard a rumor that it is around $12,000.
2(42000)+12000= year 1 DNP + year 2 DNP + last semester of DNP = $96,000
Overall Cost:
So total tuition for MDE and DNP= 113211 + 96000 = $209,211. Reminder that this is only the tuition. With housing, transportation, health insurance, other academic fees, and general cost of living for about 3 years added onto the MDE+DNP tuition, you’re looking at a price tag of at least $250,000.
***Scholarships, need-based aid, and loans have not been deducted from these calculations as these will vary by student.
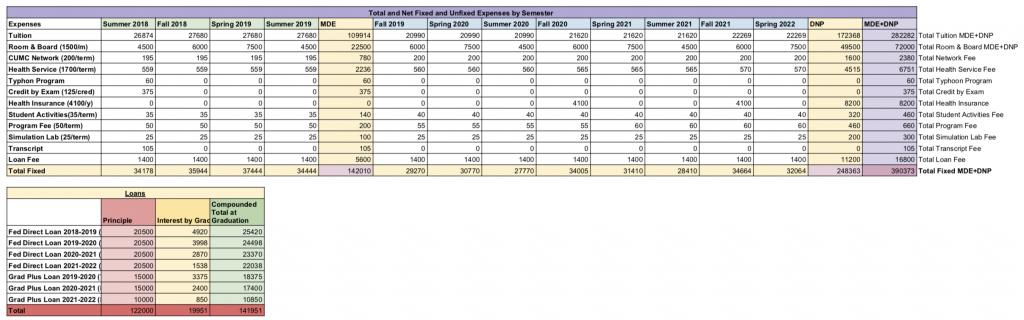
If you’re good with excel or google sheets, I recommend creating a spreadsheet to calculate projected costs. I have a complex spreadsheet that combines “fixed” costs (tuition, academic fees, housing, health insurance, ect.) and “unfixed” costs (transportation, food, gym, having a life, ect.), and subtracts any sources of “income” (scholarships, aid, loans, any monetary help from family). With costs I was unsure of (like housing), I made sure to make my estimate much higher than I was actually aiming to spend because I’d rather be plan to deal with a higher number from the beginning than be unpleasantly surprised in the future. I also have a sheet that calculates different levels of loans at different compounding interest rates. Here’s an example of something I created for fixed costs and loans (the numbers may be different b/c of changes in the program):
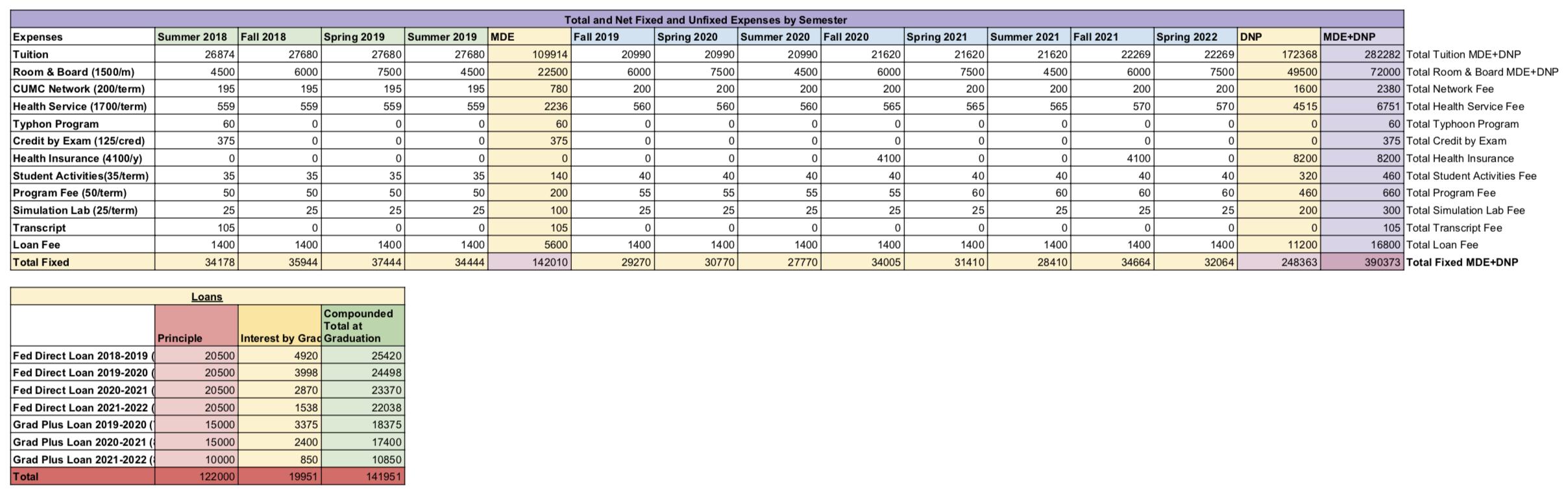
Use a spreadsheet to calculate and track costs.
At such prices, these programs are completely inaccessible to many students without the burden of taking on hundreds of thousands of dollars of student loans, which currently have 2019 interest rates of 6.6% and 7.6% for direct unsubsidized and direct PLUS loans, respectively. There are cheaper options to consider to enter into the field of nursing and work as a nurse practitioner, including programs at state schools and community colleges. However, many of these programs do not have programs for certain specialties, like psychiatric mental health. Online programs exist but I’m still a firm believer in in-person learning with the current technology that exists, especially in a dynamic and patient-centered field like nursing. Loan repayment options exist, including those through HRSA (NHSC and Nurse Corps), Public Service Loan Forgiveness, and various employer-based loan repayment options (ex. many hospitals/medical facilities/branches of the military will pay off a portion of your student loans), but I wouldn’t completely bet on any of them taking care of the study loans. Remember that the former options are competitive programs with limited funds run by government agencies that may not deliver.
The good thing is that registered nurse and nurse practitioner jobs are in high demand, offer stable salaries, and offer many ways to increase income (working overtime, working per-diem/moonlighting/locum tenens, consulting, working in a private practice, or working multiple jobs- which is easier with many nursing jobs occurring on a shift schedule).
The decision ultimately comes down to your current financial situation, how much you think this investment is worth, and how willing you are to shoulder a significant debt for a decent portion of your foreseeable future. From an optimistic viewpoint, you will make enough as a registered nurse or nurse practitioner to maintain an okay standard of living if paid off incrementally over a long-enough stretch of time, or enough to live bare-bones and aggressively pay off the loans over a shorter period of time. However, if the thought of carrying debt for a long period of time, or sacrificing quality of life for a shorter period makes you extremely anxious/stressed and keeps you from investing emotionally/financially into creating a life that will make you happy, this may not be the route for you.
Overall Pro’s:
These are what I think makes Columbia’s MDE and DNP programs strong:
- Great clinical placements/clinical connections. See clinical section above.
- Seamless direct-entry MSN to DNP pathway. As someone with a bachelors in a field other than nursing who is certain about the NP specialty I want to go into, this is a great option to save myself time (if not money lol) and get all of my formal education out of the way in one go. This program also appealed to me because it is the only direct-entry nursing program in which you seamlessly earn a Master’s and Doctor of Science in Nursing. In many other programs in the same amount of time (2-4 years), you receive a BSN and MSN, with a DNP requiring further investment (both financial and time). Currently with Columbia’s MDE-DNP route, students can receive a MSN and DNP within 3-3.5 years total (except for acute where you need to take a year in-between to gain clinical experience). While many NP’s practice with an MSN, I want to invest in getting a DNP for a few personal reasons:
- I want to work in higher-education at some point in my career, so it would be helpful to have a doctoral degree.
- I want to go into policy work at some point in my career and having a doctoral degree may open some doors/help me gain a seat at some tables.
- I want to be in leadership positions from which I can translate research findings into clinical practice. A DNP will be helpful in reaching leadership positions.
- I want my terminal degree in a field. Although I do not believe that having certain letters in front of or behind one’s name signifies greater value or competence in life, there’s a certain sense of satisfaction that comes with getting a terminal degree in any field because doing so takes time, dedication, and mastery of a certain set of knowledge/skills.
- Location: See the location section above. Even if New York City isn’t where you want to work/live for a long period of time, there is such a diverse array of people, places, and environments in and around New York that I feel like living in NYC for even a short period of time is like taking an accelerated course on life.
- The DNP programs seem strong. Students I’ve heard from in the DNP programs seem pretty satisfied, and it seems like there is a strong clinical focus in each program. I was looking for a strong psych DNP program and it seemed like Columbia had one that had an emphasis on psychotherapy and holistic treatment in conjunction with comprehensive training in psychopharmacological treatments.
- Convenient public transportation. With the subway system, public busses, Columbia’s intercampus shuttles, and Uber/Lyft/Via if all else fails, you will probably never need a car to get to clinical or class as a student living in or near Manhattan.
- The CUSON facilities. Columbia School of Nursing has a beautiful new building completed in 2017 with state-of-the-art simulation labs, medically accurate examination rooms, and study space to take advantage of. Being in the first cohort of students to be able to take advantage of these facilities, I’ve been able to practice nursing skills on mannequins that blink, breathe, speak, and even give birth! Being able to practice clinical skills and role-play clinical scenarios (and watch/receive feedback on recordings afterward) help us feel more prepared when we encounter those situations with real patients.
- The students. I have found each of the students that make up my student cohort to be rich, talented, caring, and passionate individuals. One of my favorite things that some instructors have students do at the beginning of a new class or clinical rotation is to have all of the students play ice-breaker games. People come from such different backgrounds, age ranges, life stages, hometowns, professional experiences, academic pursuits, hobbies, ect. According to the 2018-2019 statistics, the average age of students in CUSON is 27, with an age range of 21-71. That accurately reflects my experience with my cohort. There are students who started the program just after graduating from undergrad, students who have a few years of work experience, students who have had full careers in other fields, and students who have families or have started families.
- Affiliation with Columbia University. You get access to all of Columbia University’s shared resources, including the various libraries, access to events hosted by the university, and a large and strong alumni network.
Overall Con’s:
Every nursing program will have its issues and areas it can improve on. Here are CUSON’s shortcomings from my perspective in the 2018-2019 MDE cohort:
- Disorganization of the MDE program. My MDE cohort started around 230 students. The logistics of teaching so many students and coordinating with dozens of health care administrations for clinical rotations all over New York gets messy. Because of that, it sometimes feels like the program is disorganized, with last-minute changes and announcements popping up in your email on biweekly basis. The way instructors organize their material and communicate with students could be more uniform- I’ve often had to look in several different places for announcements/materials from each instructor (outlook email, Canvas inbox, Canvas announcements, Canvas files, Canvas modules).
- MDE Classes are long, and some aren’t engaging. Because we need to fit in clinical hours while squeezing in all of the nursing curriculum, we have long classes. The short classes are 3 hours long! Longer classes are 4-5 hours long. Often times, you have 2-3 classes a day, 3-4 days a week. That’s a long time to focus, take notes, and be seated- and this doesn’t account for when you do work/study on your own later on. These are the sacrifices you make for condensing the curriculum/clinical hours into a 15 month time span. There are programs that condense it into even shorter timespans, but there are also programs that spread it out over a longer time span. Also, the larger classes (foundational classes taught in the summer and other master’s classes) that are taught to the whole cohort are hard for both professors and students because of the size of the class. How engaging can a class be when it’s taught in a large lecture hall to 230+ students? Classes get much better during the 5 by 5 rotations when professors are teaching in smaller classrooms to 40-50 students. Some classes are definitely “fluff” classes. They cover important topics and concepts but are hard to teach well due to the general nature of the subjects covered and due to the class-size problem just covered. It’s frustrating to pay tuition for these classes, but they do offer respite from an otherwise grueling curriculum.
- The MDE program is relatively new and is constantly evolving. This is a good and bad thing. For the program to improve, it has to change. However, because Columbia transitioned from its Entry to Practice (ETP) (accelerated BSN) program to its MDE program relatively recently in the summer of 2016, kinks are still being worked out. I’ve heard from students in the two classes above mine (2016 and 2017) that they felt a bit like guinea pig’s with all the improvements they felt like the program had to make based on their feedback. The good thing is that it seems like the administration does take feedback seriously and make changes based on that feedback. However, because many changes are being made, the next class is often the first class to experiment with the change and that can be a bit of a bumpy ride. Examples of changes that I’ve heard occurred include how much med-math was included in the curriculum, how much evidence based practice was in the curriculum, and how skills and simulation labs are carried out.
- This is an expensive program in an expensive city. See the cost section.
This is just my personal opinion of Columbia School of Nursing’s Master’s Direct Entry and Doctor of Nursing Practice programs having gone through 8.5/15 months of the MDE program from 2018-2019. Everyone is different and I have friends who like the program much more than I do, as well as those who dislike the program much more than I do. If anything is inaccurate and/or you have any feedback/things to add, please let me know- I would love to improve this article!




This is perfect for mybuddies on LinkedIn-shared!|